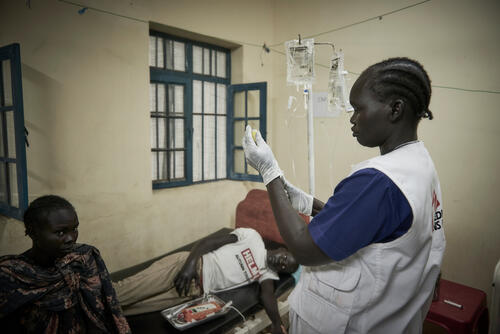
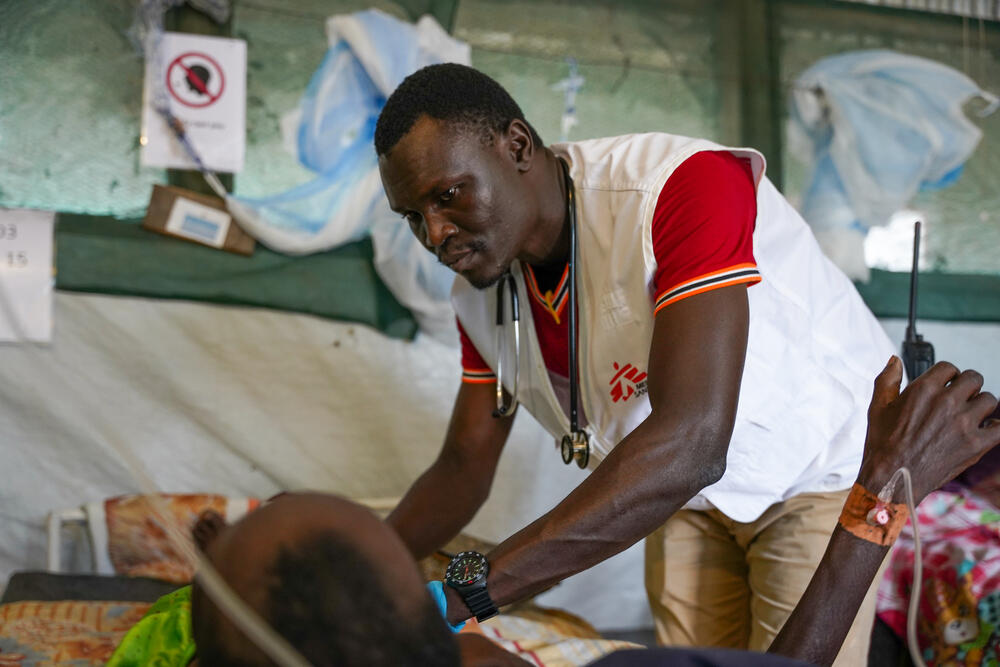
Snakebite
Snakebite is a hidden health crisis that kills more than 100,000 people a year.
Although the exact number of global snakebites is unknown, estimates put the number of people bitten by venomous species at 2.7 million a year.
Of these, some 400,000 will require an amputation or be left with another type of permanent disability. In sub-Saharan Africa alone, an estimated 20,000 people die from snakebites each year.
MSF is campaigning to improve access to more effective and affordable antivenom – a major barrier to improving survival rates.
We cared for 6,500 people who suffered snakebites in 2019.
Spotlight: Sub-Saharan Africa
100,000
PEOPLE KILLED BY SNAKEBITE EACH YEAR
400,000
REQUIRE AMPUTATION FOLLOWING SNAKEBITE EACH YEAR
6,500
PEOPLE TREATED FOR SNAKEBITE BY MSF IN 2019
Guide to snakebite
Most people bitten by snakes live in tropical or subtropical countries where venomous species are endemic. Those most at risk include agricultural workers, children and rural communities.
The highest number of cases seen by MSF are in Central African Republic, South Sudan, Ethiopia and Yemen.
However, in many affected counties, access to appropriate medical care can be restricted by:
- A lack of effective or affordable antivenom
- Limited training for medical staff
- An absence of ambulance services to rapidly transport patients to hospital
- Distrust in antivenom due to low-quality products on the market
Following the request from UN member states, the World Health Organisation (WHO) classified snakebite envenoming as a highest priority neglected tropical disease in June 2017.
The venom from a snakebite is often unique to the species of snake involved. However, three main conditions generally result from the different venoms:
Cytotoxic venom attacks the body’s cells
- This causes rapid and painful swelling that can progress into necrosis, meaning tissue around the bite can die off irreversibly. Entire limbs can be affected and it is particularly dangerous when a patient’s airway swells.
Haemotoxic venom causes bleeding that fails to clot
- This means prolonged bleeding from the bite itself, as well as other wounds or the gums and mouth. In more serious cases, patients can experience spontaneous bleeding, shock and convulsions.
Neurotoxic venom affects the central nervous system
- This can cause numbness, excessive sweating, salivation and a strange taste in the mouth, followed by droopy eyelids and problems speaking. In severe cases, patients may experience lockjaw, breathing difficulties and eventual paralysis, leading to respiratory failure as the muscles responsible for breathing stop working.
Venoms can also cause low blood pressure, increased heart rate, upper-back pain, vomiting and diarrhoea.
The initial sign of a snakebite is a bite, often to the arms or legs, with two distinct puncture wounds from the animal’s fangs.
Ideally, medical staff should quickly determine the species of snake involved. This will decide the type of treatment required.
However, identifying the exact species can often be difficult.
The use of antivenom – an antidote to snake venom – is the most reliable treatment for snakebite. In some cases, it is the only way to prevent death.
In 2017, MSF admitted more than 3,000 patients to its clinics for snakebite, predominantly in sub-Saharan Africa and the Middle East. Around half of these people required antivenom treatment, which MSF provides free of charge.
Treating, diagnosing and preventing snakebites is a focus for our teams working in Ethiopia's Amhara region.
In 2018, our clinic in Abdurafi treated 647 patients for snakebites. As well as caring for patients, we are also trying to find a more effective snakebite treatment.
Why is snakebite still devastating families?
Limited access to quality antivenom is the biggest obstacle to surviving a snakebite:
- In remote, rural locations, medical care may be several hours away while stocks of antivenom can be non-existent
- In some regions, available medication is often ineffective or non-specific to common snakes in the region
- Low-quality antivenom can trigger life-threatening side effects such as anaphylaxis, an extreme allergic reaction
For these reasons, MSF projects in affected areas carry stocks of high-quality antivenoms that are appropriate for the range of native species.
The high cost of antivenom is a major barrier to people accessing treatment.
The expensive price for the required number of doses can drive entire families into debt, forcing patients to cut short their treatment. They may then try cheap but low-quality antivenom or visit untrained traditional healers – putting their health at further risk.
This results in a vicious circle: High prices drive people to use low-quality antivenom, causing them to lose confidence in the medication altogether. This creates a drop in demand which means quality suppliers either raise their prices further or stop production altogether.
In May 2019, MSF welcomed the release of a long-awaited WHO strategy on the prevention and control of snakebite envenoming, which commits to halving the number of snakebite deaths and cases of disability by 2030.
The WHO plans to achieve this through four key objectives: empower and engage communities; ensure safe, effective treatment; strengthen health systems; and increase partnerships, coordination and resources.
Snakebite: News and stories